
Farm Tours
We offer farm tours for smaller groups and families to meet, feed, interact with and walk with our alpacas.
For full details and to book your experience of these wonderful animals, please go to our reservation form.
Alpacas are stoic and often hide signs of illness. All owners should know the normal behaviour of their animals so that early recognition is easier. The following may indicate a problem:
This guide outlines the commoner alpaca illnesses in New Zealand, how to recognise them and when to seek veterinary advice.
Worms and other parasites affecting alpacas are now found on this page and given the importance to alpacas, Facial Eczema has its own page.
If you cannot find what you are looking for on this page, I would really appreciate a note to tell me so that I can write on the subject for you and future visitors.
With appropriate care, alpacas maintain very good health. As with all livestock, occasional health issues are found and this page may help the reader to recognise these.
Please note:This information is provided only as a guide to the commoner illnesses in alpacas. If an owner cannot quickly determine the cause of any abnormal symptoms or behaviour by an animal, veterinary assistance must be sought. Nothing provided here is a substitute for veterinary consultation.
Drug treatment of alpacas is well established and veterinarians routinely manage a wide range of conditions successfully. As few medicines are specifically licensed for camelids, they are used "off label", meaning they are not formally approved for alpacas but are known to be safe and effective in practice. Dosage is typically based on veterinary experience and established use in similar livestock such as sheep.
Alpacas will graze a wide variety of plants but many found growing in New Zealand paddocks and gardens are poisonous to livestock and must be removed if within reach. There is a saying of "if in doubt, pull it out" for good reason. Crias are most at risk as they will try plants that the adults avoid.
The list of toxic plants is extensive but perhaps the most likely encountered in New Zealand would be Oleander, Foxglove, Hemlock, all Nightshade members, Laburnum, Iris, Jerusalem cherry, Rhododendron, and Azalea, Ragwort, and Box hedging. Of these, hemlock and rhododendron/azalea are the most dangerous as they are relatively common, and ingestion of even small quantities of any parts of the plant can be fatal. If an owner believes that an animal has eaten any of these, veterinary help must be obtained immediately.
This page shows a photograph gallery of toxic plants that grow in New Zealand and other countries.
Vitamin D is synthesised in the skin through a chemical reaction caused by ultra-violet (UV) radiation. As alpacas evolved at high altitude where they are exposed to high intensities of UV radiation, when they are kept at low altitudes, the amount of UV radiation received is lower and they may become vitamin D deficient. Alpacas younger than 2 years old along with pregnant or lactating females are most at risk of deficiency. Low sunshine hours and animals in full fleece are at particular risk.
Vitamin D is responsible for the effective absorption of calcium, magnesium and phosphate and is also involved in the regulation of calcium levels in the bloodstream. Any deficiency will therefore affect the growth or/and calcification of bones. The deficiency condition is called rickets in young animals but osteomalacia/osteoporosis in adults.
Rickets is commoner in crias unpacked later in the year and to darker fleeced animals. Symptoms may include lethargy, being reluctant to walk and when moving show a splay-legged gait, have a hunched back and bowed fore-limbs. Veterinary consultation is vital as failure to treat will result in permanent deformation of the bones. As always, prevention is the best course and is discussed in this section on injection schedules.
Osteomalacia involves removal of calcium and phosphate from the long bones. Symptoms are similar to rickets and can also be treated under veterinary supervision with vitamin D and phosphate supplements.
This skin condition is familiar to many livestock owners and is known by many names: 'cutaneous streptothrichosis' (cattle, goats, and horses), 'rain-scald', ‘mud rash’ or 'mud fever' (horses), 'lumpy wool' (sheep), 'strawberry foot rot' (sheep and cattle) and is a causative factor in 'pastern dermatitis' (horses). It is caused by the bacterium Dermatophilus congolensis and can result in severe skin infections indicated by the formation of crusty scabs containing the microorganism. In alpacas, these lesions are most common on the back and wet, clumped wool may be found that is removable in clumps. The underlying skin is often reddened and weeping.
The bacterium exists in two forms: filamentous and motile zoospores. The zoospore is resistant to heat and being dried out and as it is the dormant phase, it can survive in infected scabs for months. Transmission between animals is known to occur by direct contact but contaminated environments may also be an indirect means.
Veterinary consultation is essential as the treatment will include antibiotics - fortunately the bacterium is sensitive a wide range. Povidone iodine shampoos or chlorhexidine solutions are also useful in clearing up the disease.
This is a condition caused by the endophyte fungus Epichloë festucae (var. lolii) which is found in the leaf sheath of perennial ryegrass pastures. The endophyte is a deliberate addition to the ryegrass seeds to deter insects, particularly the Argentine Stem Weevil, and increase grass growth rates. The condition is particularly common in New Zealand, possibly due to the combination of endophyte-infected ryegrass and the practice of monoculture. This fungus produces several mycotoxins including lolitrem-B, peramine and ergovaline which when ingested cause neurological symptoms [5]. The disease usually occurs in mid/late summer and autumn or after a drought when new grass is growing quickly. This condition mainly affects animals under 2 years of age but only some are affected, suggesting a genetic predisposition and these may be permanently at risk.
In its mildest form, there are slight head tremors or head wobbling but the animal will often appear normal until it becomes excited or agitated. If left untreated, the condition progresses to head shaking, showing a high-stepping gait and a stiffness that can lead to poorly coordinated walking (ataxia). Later there may be complete loss of limb control and the animal will be prone to falling over. Once removed from the pasture, most animals will recover with no apparent residual effects. To achieve this, the patient should be stabled with another alpaca and provided with alternative feedstuffs such as hay, chaff and kibble. The recovery time is between one and three weeks. Veterinary treatment may include an injection with vitamin B1 to eliminate the possibility of polioencephalomacia (thiamine deficiency), which exhibits similar symptoms.
Tuberculosis is an infectious disease caused by the bacterium Mycobacterium bovis. It can affect a wide range of animals in New Zealand but cattle and deer are most at risk of contracting the disease. The common brushtail possum (Trichosurus vulpecula) is the main wildlife vector (carrier) of bovine Tb in New Zealand. This animal was introduced from Australia for the production of its fine fur. However, it is now endemic and estimates of numbers are certainly greater than 50 million. This possum is also responsible for significant damage to forests and the killing of native wildlife. The usual route of Tb infection is through the inhalation of droplets expelled from the lungs of an infected vector.
The TBfree programme (through OSPRI) aims to eradicate bovine Tb from New Zealand through targeted control. As part of the process, the country is divided into Tb control areas with each having a specific testing frequency and movement control measures, depending on the risk of Tb transmission from an infected vector.
As it is now established that camelids are susceptible (if resistant) to this disease, the AANZ has set up a procedure for testing and reporting of camelid herd Tb status. The scheme is voluntary but all owners are strongly recommended to take part. Moreover, it is currently a condition of attendance at A&P shows that alpacas are tested and have valid certificates. All herd members over 6 months old must be tested to gain a “Whole Herd” status.
The single tuberculin test (STT) is approved for use as a primary Tb test for alpacas. An accredited vet will need to apply the test to an area of skin either at the neck site (about level with the animal’s back) or behind the foreleg. The neck site is the AANZ preferred and recommended site. Examination of the test site is made two or three days later for any skin reaction.
A detailed Tb reference card from the AANZ archive can be downloaded.
Johne’s disease is one of global significance. Simply from an economic loss standpoint, it is prominent among rumunant species, cattle, sheep, deer and goats with many herds having infected animals. Furthermore, the wider range of species that can be infected is illustrated by a review of published data on affected zoo animal species [50], which included alpacas and llamas.
The disease is caused by the bacterium Mycobacterium avium ssp paratuberculosis and results in a very gradual thickening and inflammation of the intestinal wall (enteritis) which eventually prevents the absorption of nutrients. Infection most commonly occurs at a young age through ingestion of the bacteria but symptoms are not seen for some years. The shedding of bacteria in the faeces starts before there are any clinical signs thus is the main source of transmission between animals. The bacterium survives for long periods in the paddock.
Clinically, Johne’s disease is characterised by slower growth rates in younger animals but as the disease advances there will be weight loss and often profuse diarrhoea. Affected animals eventually die. A diagnosis may be confirmed by various testing methods. Growth of M. avium bacteria from faecal samples is possible but is a slow process due to the slow growth rate of the organism. There are currently no treatments for Johne's disease.
In New Zealand, Dairy NZ has produced a Johne’s Disease guide containing tools to combat the infection and prevent its spread in herds. A vaccine is available for sheep and goats but not cattle due to the interference of the vaccine with TB testing. This would also be an issue with alpacas being taken to shows as a clear TB status is currently required.
Alpacas kept in damp or even wet paddocks may develop pododermatitis. This can be seen as blisters and sloughing from the footpads and often there are infections caused by anaerobic bacteria, frequently Fusobacterium necrophorum [34]. Veterinary treatment involves the removal of damaged tissue, antiseptics and possible use of foot protection to allow healing. Antibiotics are often given. Growth of new tissue on the footpad may take many weeks and is helped by keeping the animal in a dry environment.
Given their high fibre diet, it might seem counter-intuitive that alpacas can suffer from constipation. The cause may be unclear but possibilities are a sudden change of diet, drinking too little water or even stress. Symptoms include an increased frequency of rolling, increased vocalisation, laying on one side and kicking at the stomach, all of which suggest abdominal pain.
Veterinary assistance is needed as treatment may include Buscopan (smooth muscle relaxant), Flunixin (Banamine) for pain relief and mineral oil administered either orally or rectally. Walking the alpaca on a halter and lead will assist the action of the oil. Faecal material is usually expelled after a few hours and often as large masses. Normal defecation resumes within 24 hours.
Most alpaca owners will have seen an alpaca with diarrhoea at some point. Unfortunately there are many causes and detective work can eliminate some possibilities before the arrival of the vet. Diarrhoea must be taken seriously as the alpaca can lose significant amounts of water and electrolyte as a result.
Following are a number of possibilities:
The ability of alpacas to survive and thrive at altitude and at temperatures between -15℃ and 40℃ make them versatile animals from the human perspective. However, higher temperatures and humidities can be an issue if the alpaca is in full fleece, a situation made worse if it obese. Heat Stress is less likely in New Zealand but a significant risk in many other countries that alpacas are now raised in.
Symptoms may include abnormally rapid breathing through an open mouth, shaking and foaming at the mouth. The body core temperature is significantly raised. Should these symptoms be seen, veterinary help should be called in but the animal should have its body fleece removed immediately. Water can then be used to cool the alpaca but other measures can be used by the veterinarian.

Choke in alpacas is often associated with the rapid consumption of pellets (kibble). Symptoms may include abnormal regurgitation sounds, copious salivation/drooling and saliva/pellet mixture being expelled from the mouth (see image). Rapid pellet consumption may be due to an animal gaining access to a feed bag of the kibble, a dominant animal eating multiple portions or a low-ranking animal quickly grabbing and swallowing what they can get.
The blockage can occur anywhere along the length of the oesophagus which is about 1.2 meters long in the adult. Some alpacas will clear the blockage themselves though in milder blockage cases, gentle upward massaging of the oesophagus may relieve the obstruction if it can be located. However, should the blockage be cleared quickly, veterinary help must be obtained as other treatment methods are available but these may require sedation. Critically, any alpaca that has completely blocked the oesophagus will start to bloat as it cannot expel gasses from its rumen fermentation.
Choke is completely preventable by mixing the kibble in with chaff. Doing this makes the alpaca search for the kibble pieces and because its eating is slowed down, enough saliva is produced to lubricate the chewed kibble down the oesophagus normally.
Note that pieces of carrot or apple should always be offered one at a time. Some alpacas are overly enthusiastic when being hand fed and may take several pieces at once. Because alpacas cannot easily chew large or multiple chunks, these may be swallowed whole. When this happens, the pieces can become lodged in the oesophagus, not fully blocking it but preventing normal swallowing. An affected alpaca will usually stop eating immediately and may make audible gurgling or gulping sounds as saliva accumulates and attempts to clear the obstruction. Gentle massage of the neck along the line of the oesophagus may sometimes help move the food down into the stomach. However, if the obstruction does not clear quickly, or the animal appears distressed, immediate veterinary attention is essential to prevent complications.
Tooth root abscesses are relatively common in adult alpacas. They usually affect the molar teeth in the lower jaw (mandible) although upper molars can also be involved. The condition results due to bacteria entering the tooth's root, often through tooth wear, fractures in a tooth, poor jaw alignment, food impaction or periodontal disease.
Typical signs include:Prevention focuses on good dental management. Ideally, a regular inspection of the teeth (especially in older animals) should be done but in practice, this can be difficult. In particular, owners should ensure that any supplementary feeds given are not contaminated with stones, grit or other hard materials.

Pink eye is a painful, potentially contagious condition marked by an inflamed red conjunctiva, watery discharge, squinting and a hazy blue or white cornea. Apart from the obvious colour, the alpaca may be squinting, closing its eye(s) and avoiding bright sunlight. If any of these symptoms are seen, consult your veterinarian.
Traditional pinkeye in alpacas, sheep and goats can have an infectious cause - Mycoplasma, Chlamydophila and Moraxella are pathogenic bacteria commonly involved. However, high dust levels, crowded conditions or irritation from grass seeds or foreign objects can also trigger it. Mycoplasma and Chlamydophila are particularly difficult organisms to deal with as common eye antibiotics have poor efficacy as a treatment. Particular antibiotic treatments are needed and applied into the eye every few hours for them to work, which can be challenging as the eye area will be very sensitive. Anti-inflammatory drugs may also be given as reduced swelling will also result in less pain for the alpaca.
Infected animals should be separated from the herd to prevent transmission, ideally somewhere shaded and close to other herd members, provided it does not stress them. If the alpaca is halter trained, it should be led there. Given that the animal may be almost blind, herding it into the yard is not recommended as it may not see fences or gateways and injure itself running blindly. They should have free access to hay and baleage.
Alpacas can develop cataracts exactly like humans, dogs and horses. A cataract is a clouding of the eye’s lens that interferes with light passing through to the retina. The opaque lens causes a degree of visual impairment, rangeing from blurry vision to visual blindness.
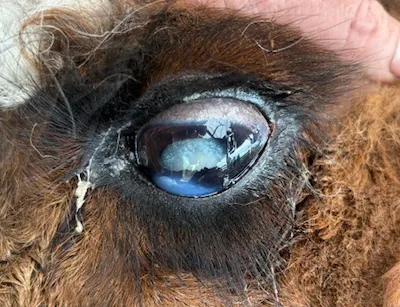 Examination of an animal may show:
Examination of an animal may show:
Diagnosis should be made by a vet who will examine the eye with an ophthalmoscope. Treatment depends on the age of the animal and the severity. Monitoring the eye for any deterioration appears common - in a young animal there may not be progression and in older ones, surgical procedures may not be attractive as removal/replacement of the lens can be expensive. Older alpacas adapt well as they can rely on their hearing, smell and the herd behavior. However, it is necessary to ensure that they stay with their usual herd companions, the pasture layout stays predictable and hazards are minimized. Any handling must be kept calm.
 Quidding refers to the habit of dropping wads of partially chewed material instead of swallowing it or packing these wads into the cheek. While more commonly seen in horses, quidding in alpacas is an important sign of mouth pain, dental disease or jaw problems. Observing feeding behaviour is one of the best ways to detect these issues and you should seek veterinary assistance if you notice any of the following symptoms:
Quidding refers to the habit of dropping wads of partially chewed material instead of swallowing it or packing these wads into the cheek. While more commonly seen in horses, quidding in alpacas is an important sign of mouth pain, dental disease or jaw problems. Observing feeding behaviour is one of the best ways to detect these issues and you should seek veterinary assistance if you notice any of the following symptoms:
Although less frequent than in other species, alpacas can develop gum inflammation or periodontal disease, especially if dental problems go untreated. Infection around tooth roots is a major cause of chronic quidding.
Sometimes quidding is encouraged by overly coarse or stemmy hay or hard pellets. While not a root disease, poor-quality feed can aggravate existing dental issues and increase the likelihood of quidding.
Most of the literature below can be accessed by clicking on the highlighted link. Some links will access the appropriate web page from which the article can be downloaded but others will immediately start downloading the full reference.
5. Philippe, G. (2016). Lolitrem B and Indole Diterpene Alkaloids Produced by Endophytic Fungi of the Genus Epichloë and Their Toxic Effects in Livestock. Toxins (Basel), 8(2): 47. DOI: https://doi.org/10.1038/ncomms2516
20. Foster, A. (2008). Skin diseases of South American camelids. Br. Vet. Zool. Soc. Proc., May: 30-32.
34. Kumar, A., Anderson, D., Amachawadi, R.G., Nagaraja, T.G. and Narayanan, S.K. (2013). Characterization of Fusobacterium necrophorum isolated from llama and alpaca. J. Vet. Diag. Invest., 25(4): 502–507.
49. McCaslin, E. (2009). Mighty Mites: Chorioptic Skin Disease in Alpacas. Alpacas Magazine, Herd Sire, 150-155.
50. Roller, M., Hansen, S., Knauf-Witzens, T., Oelemann, W., Czerny, C. P., Abd El Wahed, A., and Goethe, R. (2020). Mycobacterium avium ssp paratuberculosis Infection in Zoo Animals: A Review of Susceptibility and Disease Process. Front. Vet. Sci., 7, 572724.
72. Van Saun, R.J. (2009). Nutritional diseases of llamas and alpacas. Vet. Clin. Food Anim., 25: 797-810. doi:10.1016/j.cvfa.2009.07.013